Articles
Article Tools
Stats or Metrics
Article
Original Article
Exp Neurobiol 2019; 28(4): 458-473
Published online August 31, 2019
https://doi.org/10.5607/en.2019.28.4.458
© The Korean Society for Brain and Neural Sciences
Increased CD68/TGFβ Co-expressing Microglia/ Macrophages after Transient Middle Cerebral Artery Occlusion in Rhesus Monkeys
Hyeon-Gu Yeo1,2†, Jung Joo Hong1†, Youngjeon Lee1,2†, Kyung Sik Yi3, Chang-Yeop Jeon1, Junghyung Park1, Jinyoung Won1, Jincheol Seo1,4, Yu-Jin Ahn1,2, Keonwoo Kim1,5, Seung Ho Baek1, Eun-Ha Hwang1,6, Green Kim1,6, Yeung Bae Jin1, Kang-Jin Jeong1, Bon-Sang Koo1, Philyong Kang7, Kyung Seob Lim7, Sun-Uk Kim2,7, Jae-Won Huh1,2, Young-Hyun Kim1,2, Yeonghoon Son8, Ji-Su Kim8, Chi-Hoon Choi3, Sang-Hoon Cha3* and Sang-Rae Lee1,2*
1National Primate Research Center, Korea Research Institute of Bioscience and Biotechnology (KRIBB), Cheongju 28116, 2Department of Functional Genomics, KRIBB School of Bioscience, Korea University of Science and Technology, Daejeon 34113, 3Department of Radiology, Chungbuk National University Hospital, Cheongju 28644, 4School of Life Sciences, BK21 Plus KNU Creative BioResearch Group, Kyungpook National University, Daegu 41566, 5Department of Physical Therapy, Graduate School of Inje University, Gimhae 50834, 6Laboratory Animal Medicine, College of Veterinary Medicine, Chonnam National University, Gwangju 61186, 7Futuristic Animal Resource & Research Center, KRIBB, Cheongju 28116, 8Primate Resource Center, KRIBB, Jeongeup 56216, Korea
Correspondence to: *To whom correspondence should be addressed.
Sang-Rae Lee, TEL: 82-43-240-6316, FAX: 82-43-240-6309, e-mail: srlee@kribb.re.kr
Sang-Hoon Cha, TEL: 82-43-269-6473, FAX: 82-43-269-6479, e-mail: shcha@chungbuk.ac.kr
†These authors contributed equally to work.
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License(http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, andreproduction in any medium, provided the original work is properly cited.
Abstract
The function of microglia/macrophages after ischemic stroke is poorly understood. This study examines the role of microglia/macrophages in the focal infarct area after transient middle cerebral artery occlusion (MCAO) in rhesus monkeys. We measured infarct volume and neurological function by magnetic resonance imaging (MRI) and non-human primate stroke scale (NHPSS), respectively, to assess temporal changes following MCAO. Activated phagocytic microglia/macrophages were examined by immunohistochemistry in post-mortem brains (n=6 MCAO, n=2 controls) at 3 and 24 hours (acute stage), 2 and 4 weeks (subacute stage), and 4, and 20 months (chronic stage) following MCAO. We found that the infarct volume progressively decreased between 1 and 4 weeks following MCAO, in parallel with the neurological recovery. Greater presence of cluster of differentiation 68 (CD68)-expressing microglia/macrophages was detected in the infarct lesion in the subacute and chronic stage, compared to the acute stage. Surprisingly, 98~99% of transforming growth factor beta (TGFβ) was found colocalized with CD68-expressing cells. CD68-expressing microglia/macrophages, rather than CD206+ cells, may exert anti-inflammatory effects by secreting TGFβ after the subacute stage of ischemic stroke. CD68+ microglia/macrophages can therefore be used as a potential therapeutic target.
Graphical Abstract
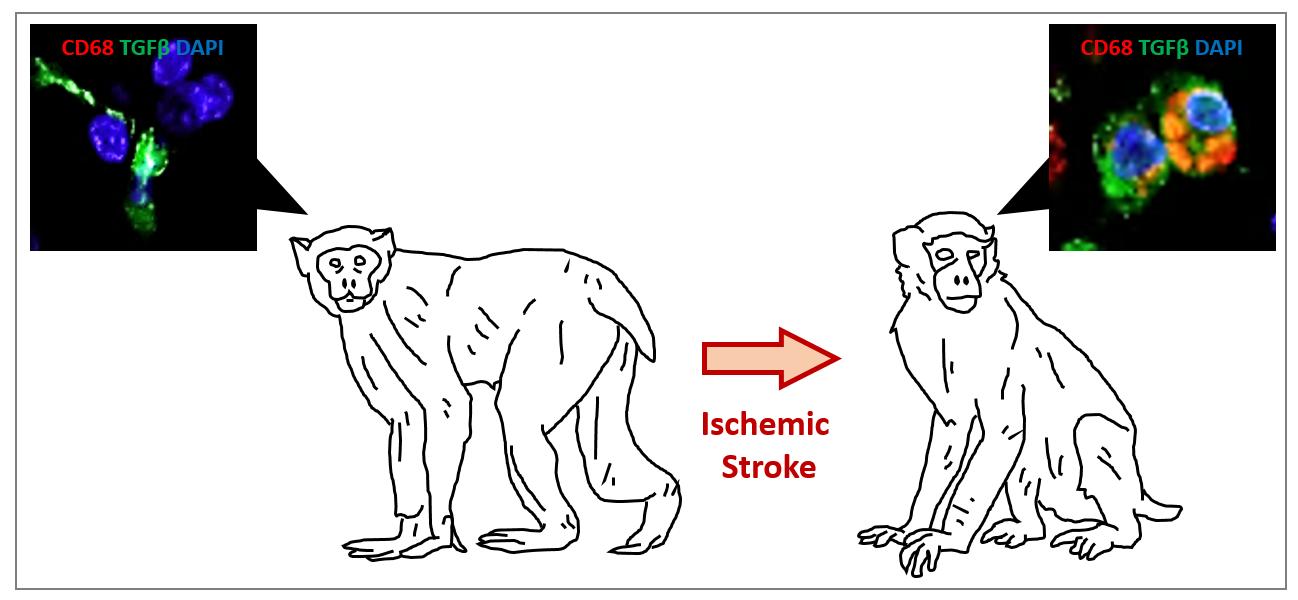
Keywords: Inflammation, Microglia, Stroke, Macaca mulatta, Transforming growth factor beta


