Articles
Article Tools
Stats or Metrics
Article
Original Article
Exp Neurobiol 2017; 26(2): 97-103
Published online April 30, 2017
https://doi.org/10.5607/en.2017.26.2.97
© The Korean Society for Brain and Neural Sciences
Optogenetic Rescue of Locomotor Dysfunction and Dopaminergic Degeneration Caused by Alpha-Synuclein and EKO Genes
Cheng Qi1, Scott Varga1, Soo-Jin Oh2,3, C. Justin Lee3 and Daewoo Lee1*
1Neuroscience Program, Department of Biological Sciences, Ohio University, Athens, OH 45701, USA, 2Convergence Research Center for Diagnosis, Treatment and Care System of Dementia, 3Center for Neuroscience, Center for Functional Connectomics, Korea Institute of Science and Technology (KIST), Seoul 02792, Korea
Correspondence to: *To whom correspondence should be addressed.
TEL: 1-740-597-1926, FAX: 1-740-593-0300
e-mail: leed1@ohio.edu
α-Synuclein (α-Syn) is a small presynaptic protein and its mutant forms (e.g. A53T) are known to be directly associated with Parkinson's disease (PD). Pathophysiological mechanisms underlying α-Syn-mediated neurodegeneration in PD still remain to be explored. However, several studies strongly support that overexpression of mutant α-Syn causes reduced release of dopamine (DA) in the brain, and contributes to motor deficits in PD. Using a favorable genetic model
Keywords: α-Synuclein, EKO, optogenetics, Parkinson’s disease, Dopaminergic neurons, Drosophila melanogaster
INTRODUCTION
A presynaptic protein α-Synuclein (α-Syn) is known to play an important role in neuronal plasticity [1,2,3,4], but its physiological role is not completely clear yet. Ironically, the pathophysiological role of α-Syn drew intense public attention since studies revealed that mutated α-Syn genes are directly associated with PD [5]. α-Syn is also known to be a major component of cytoplasmic inclusion Lewy body, a histological hallmark of PD [5,6].
Pathophysiological mechanisms underlying α-Syn-mediated neurodegeneration in Parkinson's disease (PD) remain to be further explored. In the meanwhile, several studies strongly support that overexpression of mutant α-Syn causes reduced release of dopamine (DA) in striatum, and thus contributes to motor deficits in PD [7]. For example, overexpression of a mutant human α-Syn in mice showed reduced locomotor activity and DA release [8]. This is consistent to the fact that drugs currently used to ameliorate PD symptoms increase DA levels in the brain. A gold standard PD drug, L-DOPA is a precursor of DA [9], bypassing an enzyme tyrosine hydroxylase (TH), a limiting factor in DA synthesis. MAO-B inhibitors are also used to increase DA levels as they inhibit MAO-B, an enzyme metabolizing DA. In addition, several DA receptor agonists (e.g., bromocriptine, pramipexole) have been used to reduce PD symptoms by increasing DA signal tone [10]. Drug treatments are easy and most popular interventions for PD, but also cause severe side effects due to non-specific binding and/or off-target effects. Therefore it is necessary to develop alternative strategies to treat PD symptoms without such complications.
A popular approach to target specific neural circuits is called ‘optogenetics’. The technique involves the insertion into the genome of genes (e.g., ChR2 - channelrhodopsin 2) encoding a light-sensitive channel protein [11,12]. When expressed in the membrane of a neuron and then exposed to light of a certain wavelength (e.g. blue light - 470 nm), these channels open, letting ions pass through them. Depending on the type of channel, this can activate (e.g. ChR2) or suppress a neuron (e.g. NpHR – a halorhodopsin). Genetic tools allow for the expression of these channels in specific groups of neurons – including DA neurons involved in PD. Therefore, optogenetics can be used to selectively manipulate excitability of DA neural circuits regulating motor behavior.
In this study, we wanted to examine whether reduced DA release is enough to cause PD-like symptoms. If so, can it be rescued by non-pharmacological approach? The fruit fly
In order to decrease DA release, electrical knockout (EKO; 16) gene has been expressed specifically in DA neurons of fly larval brain.
MATERIALS AND METHODS
Flies were grown in standard cornmeal/agar media with 0.4% propionic acid on a 12-hour light/dark cycle at 25℃. Fly strains used in this study were: wild-type (Canton-S), TH-Gal4 (a gift from Dr. J. Hirsh, University of Virginia), UAS-α-Syn (A53T); TH-GAL4 (TH-A53T, a gift from Dr. L. Pallanck, University of Washington), UAS-EKO (Bloomington
Individual larvae (90~94 hours after egg-laying) were separated from the food using a 15% glucose solution and rinsed with distilled water. They were then placed on the surface of a plate of 2.5% agar mixed with 1mL India ink (to have a black background). The larvae were allowed to acclimate for 1 minute and a video was then recorded for 30 seconds at approximately 10 frames per second using a Moticam3 digital camera (Motic) and Motic Images Plus 2.0 software. The video was analyzed using the MTrack2 plug-in (from http://valelab.ucsf.edu/~nico/IJplugins/MTrack2.html) for ImageJ (from http://rsb.info.nih.gov/ij/). The path length was recorded; scores were quantified as the distance traveled per minute.
For staining the
Blue light (BL, 470 nm) for ChR2 activation was shed using a custom-built optogenetics rig [20]. A GW Laboratory DC power supply was connected to a 700 mA Buckpuck constant current generator (Luxdrive). The Buckpuck was connected via a switch to a blue LED (Luxdrive Endor Star). To prevent overheating, the LED was connected to a heat sink (Thorlabs). Larvae were exposed to blue light (BL; intensity, 1 mW/mm2), either during testing or prior to testing. For optogenetic experiments, larvae were fed with food containing 1 mM all-trans-retinal (Sigma-Aldrich). Light intensity was measured using a Sanwa Mobiken laser power meter.
It is known that overexpression of mutant α-Syn causes reduced release of dopamine (DA) in striatum [7,8], and thus contributes to motor deficits in Parkinson's disease (PD). We proposed a hypothesis that reduced excitability of DA neurons may mimic α-Syn toxicity by reducing DA release. Therefore, we chose to utilize the electrical knock-out (EKO) transgene encoding a constitutively active K+ channel [16] to suppress the excitability of
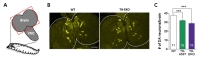
In addition to locomotion deficits, the loss of DA neurons is a key cellular hallmark of PD. Therefore, we examined whether reduced locomotion in TH-EKO is associated with reduction of tyrosine hydroxylase (TH) expression using whole-brain mounting technique [15,19]. TH is a key enzyme in DA synthesis and thus widely used as a DA marker. Our quantification of DA neurons showed that TH-EKO larvae displayed significantly reduced number of TH-positive DA neurons (Fig. 2). This reduction is slightly more severe in TH-EKO brains than TH-A53T. Along with locomotion deficits, these results clearly show that the reduced excitability in DA neurons causes PD symptoms mirroring effects of a mutant PD geneα-Syn (A53T).
Our results suggest that both α-Syn and EKO impaired DA synaptic signaling and
In the following study, we wanted to test whether the rescue of EKO effects can restore a reduced locomotion as well as a decreased TH expression level. Larvae (TH-ChR2-EKO) were driven to express ChR2 (Pulver et al, 2011) specifically in DA neurons in addition to EKO. First, blue light (BL) was shed during the locomotion test in TH-ChR2-EKO. This acute BL led the rescue of locomotion deficiency (Fig. 4), but it is likely due to enhanced DA synaptic release from existing DA presynaptic terminals, not by an increase of TH expression level. In the subsequent experiments, therefore, we looked for a long term effects of BL in order to examine TH expression. BL stimulation for 6 and 24 hours was given to TH-ChR2-EKO larvae. 6 hour stimulation was enough to rescue EKO effects but there was no rescue for 24 hour stimulation. We found that acute light stimulation during the locomotion test could restore locomotion partially (Fig. 4), whereas a long-term (6-hour) light stimulation before, but not during, locomotion test fully restored locomotion and significantly restored TH expression. These results are consistent with the idea that the reduced excitability of DA neurons causes impairment in both TH expression and motor behavior, and thus strongly reconfirm our hypothesis that reduced DA neuronal excitability can induce decrease in TH expression and locomotion defects.
Motor dysfunction in Parkinson's disease (PD) is primarily due to reduced synaptic DA release which is caused by neurodegeneration of DA neurons. A PD gene α-Syn is also known to decrease DA synaptic release [7,8]. In this study, we demonstrated that reduced excitability of DA neurons by a genetically modified K+ channel EKO [16] led to a decrease in TH signal and locomotion deficits, which mimics cellular and behavioral alterations in
Since its first use [23], optogenetic techniques have become a popular tool to precisely manipulate activities of certain neural circuits mediating normal or pathological behaviors by expressing light sensitive channels (e.g., ChR2). Indeed, it has been used to manipulate direct D1 or indirect D2 pathways in rodent basal ganglia [24]. They showed that changes in DA circuit activity can cause or rescue PD-like symptoms. Excitation of indirect D2 pathway induced a parkinsonian state while PD symptoms in 6-OHDA-treated mice were rescued by optogenetic activation of direct D1 pathway. Although
Traditionally, TH-negative antibody signal is interpreted as death of DA neurons in PD models. However, some parkinsonian symptoms are known to be reversible [27,28], suggesting that reduced DA synaptic release, but not DA neuronal loss. Our TH-EKO-ChR2 results also suggest that at least a subpopulation of DA neurons are TH-negative but still alive because DA neuronal number was increased just after 6 hour BL exposure in larvae expressing both EKO and ChR2 genes. It will be interesting to examine whether there is a reduction in other genes specifically or preferentially expressed in DA neurons such as DA transporter (DAT), vesicular monoamine transporter 2 (VMAT2) or DOPA decarboxylase (DDC) gene. DAT expression altered by α-Syn is currently controversial [7,29,30]. In addition, VMAT2 function can be interfered by α-Syn [31]. Therefore, DDC will be a useful marker to examine whether DDC(+)/TH(−) DA neurons are found in α-Syn or EKO larval brain, and thus these neurons can increase TH expression by ChR2 activation. By identifying DDC(+)/TH(−) neurons will provide new targets of PD interventions to restore DA synaptic release.



- Abeliovich A, Schmitz Y, Fariñas I, Choi-Lundberg D, Ho WH, Castillo PE, Shinsky N, Verdugo JM, Armanini M, Ryan A, Hynes M, Phillips H, Sulzer D, Rosenthal A. Mice lacking alpha-synuclein display functional deficits in the nigrostriatal dopamine system. Neuron 2000;25:239-252.
- Chandra S, Gallardo G, Fernández-Chacón R, Schlüter OM, Südhof TC. Alpha-synuclein cooperates with CSPalpha in preventing neurodegeneration. Cell 2005;123:383-396.
- Watson JB, Hatami A, David H, Masliah E, Roberts K, Evans CE, Levine MS. Alterations in corticostriatal synaptic plasticity in mice overexpressing human alpha-synuclein. Neuroscience 2009;159:501-513.
- Calo L, Wegrzynowicz M, Santivañez-Perez J, Grazia Spillantini M. Synaptic failure and α-synuclein. Mov Disord 2016;31:169-177.
- Eriksen JL, Dawson TM, Dickson DW, Petrucelli L. Caught in the act: alpha-synuclein is the culprit in Parkinson's disease. Neuron 2003;40:453-456.
- Dettmer U, Selkoe D, Bartels T. New insights into cellular α-synuclein homeostasis in health and disease. Curr Opin Neurobiol 2016;36:15-22.
- Venda LL, Cragg SJ, Buchman VL, Wade-Martins R. α-Synuclein and dopamine at the crossroads of Parkinson's disease. Trends Neurosci 2010;33:559-568.
- Yavich L, Oksman M, Tanila H, Kerokoski P, Hiltunen M, van Groen T, Puoliväli J, Männistö PT, García-Horsman A, Mac-Donald E, Beyreuther K, Hartmann T, Jäkälä P. Locomotor activity and evoked dopamine release are reduced in mice overexpressing A30P-mutated human alpha-synuclein. Neurobiol Dis 2005;20:303-313.
- Stocchi F, Olanow CW. Neuroprotection in Parkinson's disease: clinical trials. Ann Neurol 2003;53:S87-S97.
- Perez-Lloret S, Rascol O. Dopamine receptor agonists for the treatment of early or advanced Parkinson's disease. CNS Drugs 2010;24:941-968.
- Boyden ES. A history of optogenetics: the development of tools for controlling brain circuits with light. F1000 Biol Rep 2011;3:11.
- Warden MR, Cardin JA, Deisseroth K. Optical neural interfaces. Annu Rev Biomed Eng 2014;16:103-129.
- Bilen J, Bonini NM. Drosophila as a model for human neurodegenerative disease. Annu Rev Genet 2005;39:153-171.
- Whitworth AJ. Drosophila models of Parkinson's disease. Adv Genet 2011;73:1-50.
- Varga SJ, Qi C, Podolsky E, Lee D. A new Drosophila model to study the interaction between genetic and environmental factors in Parkinson's disease. Brain Res 2014;1583:277-286.
- White BH, Osterwalder TP, Yoon KS, Joiner WJ, Whim MD, Kaczmarek LK, Keshishian H. Targeted attenuation of electrical activity in Drosophila using a genetically modified K(+) channel. Neuron 2001;31:699-711.
- Schroll C, Riemensperger T, Bucher D, Ehmer J, Völler T, Erbguth K, Gerber B, Hendel T, Nagel G, Buchner E, Fiala A. Light-induced activation of distinct modulatory neurons triggers appetitive or aversive learning in Drosophila larvae. Curr Biol 2006;16:1741-1747.
- Brand AH, Perrimon N. Targeted gene expression as a means of altering cell fates and generating dominant phenotypes. Development 1993;118:401-415.
- Blanco J, Pandey R, Wasser M, Udolph G. Orthodenticle is necessary for survival of a cluster of clonally related dopaminergic neurons in the Drosophila larval and adult brain. Neural Dev 2011;6:34.
- Pulver SR, Hornstein NJ, Land BL, Johnson BR. Optogenetics in the teaching laboratory: using channelrhodopsin-2 to study the neural basis of behavior and synaptic physiology in Drosophila. Adv Physiol Educ 2011;35:82-91.
- Friggi-Grelin F, Coulom H, Meller M, Gomez D, Hirsh J, Birman S. Targeted gene expression in Drosophila dopaminergic cells using regulatory sequences from tyrosine hydroxylase. J Neurobiol 2003;54:618-627.
- Privman E, Venton BJ. Comparison of dopamine kinetics in the larval Drosophila ventral nerve cord and protocerebrum with improved optogenetic stimulation. J Neurochem 2015;135:695-704.
- Boyden ES, Zhang F, Bamberg E, Nagel G, Deisseroth K. Millisecond-timescale, genetically targeted optical control of neural activity. Nat Neurosci 2005;8:1263-1268.
- Kravitz AV, Freeze BS, Parker PR, Kay K, Thwin MT, Deisseroth K, Kreitzer AC. Regulation of parkinsonian motor behaviours by optogenetic control of basal ganglia circuitry. Nature 2010;466:622-626.
- Aumann T, Horne M. Activity-dependent regulation of the dopamine phenotype in substantia nigra neurons. J Neurochem 2012;121:497-515.
- Fossom LH, Sterling CR, Tank AW. Regulation of tyrosine hydroxylase gene transcription rate and tyrosine hydroxylase mRNA stability by cyclic AMP and glucocorticoid. Mol Pharmacol 1992;42:898-908.
- Bondon-Guitton E, Perez-Lloret S, Bagheri H, Brefel C, Rascol O, Montastruc JL. Drug-induced parkinsonism: a review of 17 years' experience in a regional pharmacovigilance center in France. Mov Disord 2011;26:2226-2231.
- Shin HW, Chung SJ. Drug-induced parkinsonism. J Clin Neurol 2012;8:15-21.
- Dauer W, Kholodilov N, Vila M, Trillat AC, Goodchild R, Larsen KE, Staal R, Tieu K, Schmitz Y, Yuan CA, Rocha M, Jackson-Lewis V, Hersch S, Sulzer D, Przedborski S, Burke R, Hen R. Resistance of α-synuclein null mice to the parkinsonian neurotoxin MPTP. Proc Natl Acad Sci U S A 2002;99:14524-14529.
- Fountaine TM, Wade-Martins R. RNA interference-mediated knockdown of alpha-synuclein protects human dopaminergic neuroblastoma cells from MPP(+) toxicity and reduces dopamine transport. J Neurosci Res 2007;85:351-363.
- Fountaine TM, Venda LL, Warrick N, Christian HC, Brundin P, Channon KM, Wade-Martins R. The effect of alpha-synuclein knockdown on MPP+ toxicity in models of human neurons. Eur J Neurosci 2008;28:2459-2473.
- Salthun-Lassalle B, Hirsch EC, Wolfart J, Ruberg M, Michel PP. Rescue of mesencephalic dopaminergic neurons in culture by low-level stimulation of voltage-gated sodium channels. J Neurosci 2004;24:5922-5930.
- Michel PP, Toulorge D, Guerreiro S, Hirsch EC. Specific needs of dopamine neurons for stimulation in order to survive: implication for Parkinson disease. FASEB J 2013;27:3414-3423.



